In my youth I worked for a paid ambulance service, and while we all lived for the emergency calls, the routine transports were the calls that paid the bills. Compared with the glamor and excitement of a lights-and-siren run to a car wreck or heart attack, transports were dull as dirt. And dullest of all were the daily runs from nursing homes to the dialysis center, where rows of comfy chairs sat, each before a refrigerator-sized machine designed to filter the blood of a patient in renal failure, giving them another few days of life.
Sadly, most of those patients were doomed; many were in need of a kidney transplant for which there was no suitable donor, while some were simply not candidates for transplantation. Dialysis was literally all that stood between them and a slow, painful death, and I could see that at least some of them were cheered by the sight of the waiting dialysis machine. The principles of how the kidneys work have been known since at least the 1800s, but it would take until 1945 for the efforts of a Dutch doctor, using used car parts and sausage casings, to make the predecessor of those machines: the first artificial kidney.
Restoring Balance
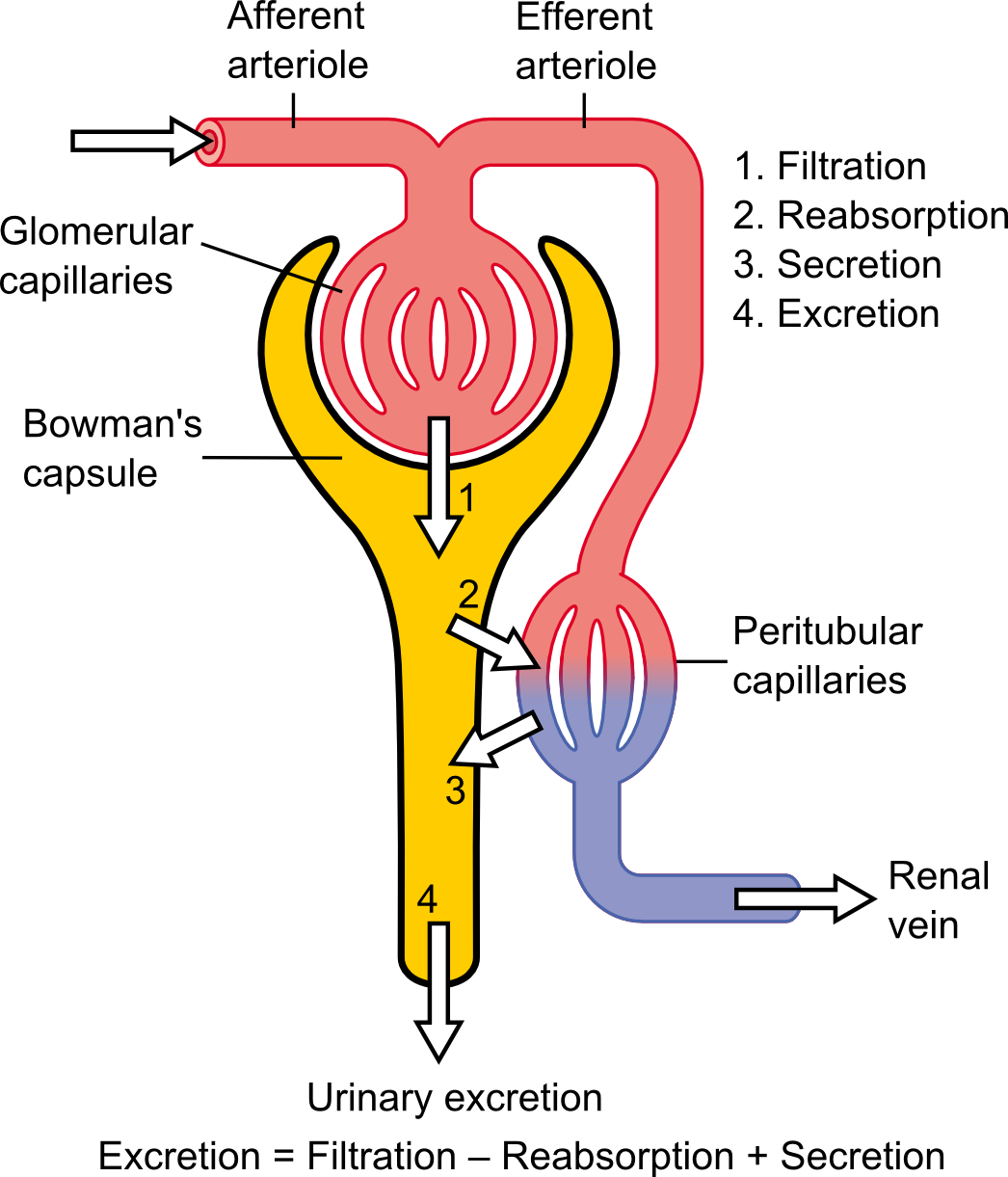
We’ve all likely seen the principle behind this demonstrated at some point in school. Osmosis is the tendency of solutions to seek a balance between solvent and solute across semipermeable membranes such as biological tissues. In the kidney, blood plasma (the solvent) containing nitrogenous waste (the solute) flows through capillaries (the semipermeable membrane). The other side of the membrane is a structure called the Bowman’s capsule, into which flows the nitrogenous waste along with a fair amount of sodium chloride, glucose, and amino acids. Most of the water and some of the solutes in that filtrate are reabsorbed by capillaries further along the Bowman’s capsule, with the balance excreted as urine.
Healthy kidneys are a marvel of efficiency, filtering the entire volume of plasma in the body 60 times a day. Of the 180 liters of the bulk filtrate produced almost all of it is reabsorbed, leaving behind about 2 liters of urine to be eliminated. Without the kidneys, the body would be unable to maintain fluid balance, blood pH, and the correct concentrations of vital electrolytes. Nausea, vomiting, and edema would follow quickly; the inevitable death would be slow and gruesome, as a young Dr. Willem Kolff would learn first hand.
No Way to Die

In 1938, a 22-year-old man entered the hospital at the University of Groningen in the Netherlands in acute renal failure. Dr. Kolff, fresh out of medical school and barely older than his patient, was put in charge of the case. There really wasn’t much to do; while Dr. Kolff knew exactly what was happening – up to 20 grams of urea were accumulating in the man’s body every day, slowly poisoning him – there was no way to remove it. Dr. Kolff could do little but watch helplessly as the man died.
Keen to find a way to save such patients, Dr. Kolff began looking for ways to “jump start” the kidneys. For several years he looked for drugs to stimulate the kidneys to improve their function, but found none. Then history took an unexpected turn and the world went to war. When the Germans swept through the Netherlands, Dr. Kolff happened to be in The Hague. As Nazi bombers swarmed overhead, he went to the hospital and volunteered to set up a blood bank. After four days of scrounging equipment and supplies and dodging Nazi snipers, the hospital’s first blood bank was in operation. It remains in operation to this day.
To avoid the worst of the Nazi occupation, he left the university hospital and headed for Kampen, a smaller city. The hospital there was glad for the help and paid the young internist enough to start working on his kidney treatments again. This time, he would concentrate on an artificial kidney.
Dr. Kolff had done experiments with cellophane sausage casings. He filled them with blood that had been spiked with urea and placed them in a saline solution. After some time and agitation, the urea had moved across the semipermeable cellophane membrane into the salt bath, removing it from the blood inside. He had the basis for an artificial kidney.
Cellophane and Salt Water
His expertise with blood banks would now come in handy. Handling blood in large volumes outside the body is not a trivial task, and doing so gave Dr. Kolff the confidence that a machine to do the job of a kidney was possible. He knew from his experiments that he’d need 10 meters of sausage casing, and that both the blood and the saline solution would need to be circulated. He built a drum from wooden slats and suspended it on an axle so that half its diameter was in a laundry tub. The cellophane tubing was wrapped around the drum and the tub was filled with saline. The tubing was filled with the patient’s blood, and a motor gently rotated the drum through the saline bath. When the blood had been cleaned, it would be returned to the patient.

The artificial kidney was crude, and initially not terribly effective. Of the first 15 patients treated with it in Kampen, only one survived, and Dr. Kolff admits she might have lived without the treatment. It would not be until 1945 that dialysis would have its first unequivocal success: a 67-year-old woman in prison for collaborating with the Nazis. Dr. Kolff was urged to let her die, but he dialyzed her and she came out of her coma. She survived for seven more years. The artificial kidney had proven itself.
Closer to the Heart

Having conquered dialysis and shared his designs freely with doctors all over the world, in 1950 Dr. Kolff was offered a job at the prestigious Cleveland Clinic. There his interests turned to other artificial organs, including the problems of open-heart surgery. At the time there was no way to bypass the heart during surgery, so he set about building one of the first membrane oxygenators, a machine that pumps blood over a porous plastic membrane to oxygenate the blood while removing carbon dioxide. This eventually let coronary artery bypass surgery become a common surgical procedure, with 200,000 performed in the United States alone every year.
Dr. Kolff also turned his inventive mind to the artificial heart. In fact, the first implantable artificial heart, the Jarvik-7, was one of Kolff’s designs. It was named after Dr. Robert Jarvik, one of Kolff’s students and the project manager on the team. In 1981 the Jarvik-7 was implanted in Barney Clark, who survived 112 days before succumbing to multiple systems failure.
Dr. Willem Kolff had a long and storied career, eventually retiring at age 86. His artificial organs, especially his artificial kidney, have saved countless lives, and continue to be used to this day. That they started with something as mundane as sausage casing and a laundry tub full of salt water only makes the achievement more impressive.
















The true spirit of “hacking”, at the best level and with the highest aim.
I hope someday I may be able to do something 1/1000 as good for mankind…
Best regards,
A/P Daniel F. Larrosa
Good Story!
Every word of the introduction fits and brought back memories. I am sure it is the same in every city. EMS: Earn Money Sleeping. I also got a lot of reading done!
A fireman/EMS told me that he had attended a training session.
During the course of the session the instructor cautioned the class, that if they are getting ready to transport the victim of a motorcycle accident, to not ask the victim if you could buy the motorcycle.
Then he said, “Wait until his wife gets to the Emergency Room, she’ll GIVE you the motorcycle!”
B^)
A couple more macabre motorcycle jokes as told by Stephen Fry: Stephen Fry interview and lap | Top Gear | BBC
We called them “donorcycles”.
I attended a medical conference a number of years ago (a guest of my wife), one of the exhibits was the development of an artificial liver. I talked with one (the?) principal researcher. It was interesting what they have accomplished, but they had so much further to go. The researcher told me they were there in hopes of finding more money for their research. At that point the apparatus could perform partial liver function for several weeks before needing “recharging”, even with partial function they hoped it could keep a patient alive until a donor could be found, with the ultimate goal of total replacement.
This would be awesome, I hope they find enough funds to develop this
Hmm, from description, it seems that, if there was a suitable healthy blood donor with matching blood groups, the healthy donor individual could have had help clean the blood of person with renal failure, by acting as this machine, getting direct transfusion from person with renal failure, and returning blood by direct transfusion back to her, all that much earlier than when the machine was invented.
There are problems with that. Main one is that white blood cells would also have ended up being transfused unless there was a way to filter them out back then, which would cause massive immune reactions after a while..
Hmm, then it is a showstopper. Filtering WBCs out, unless they are somehow returned to their respective organisms unharmed, would compromise immunities of both.
Why do I start each post with “Hmm, … “? Something is wrong with me!
Hmm …
I prescribe “The Shannon Wonder Tonic” cures all your ills or your money back.
Hmm, I hope it is not contagious!
I believe there have been cases of conjoined twins, where this principle has basically kept one twin alive when they would not have been able to survive without the “host” twin.
Before he used his prototype for the first time, Kolff tried to help his first patient with blood transfusion just to reduce the concentration of urea in blood. This helped only partially and for short time. One patient received 11 liters of blood just to keep him alive…
I can’t read this, for ten weeks earlier this year I did dialysis, three sessions of five hours each week. It was in effect an artificial kidney, though it looked like a slushy machine.
People do have to wait too long for replacement parts, sometimes too long to save them. So people should sign up to be organ donors. This is about donating if you die, so you won’t need them but it will help others. I signed up last year, expecting the worst woukd be death. But a kidney failure changed that, and I wouldn’t wish the tedium of dialysis on anyone. I was lucky, after ten weeks of it, and five sessiins if chemotherapy, my kidney is reasonably “normal” and never a word about kidney transplant.
Some teenager had a science fair project about making a dialysis machibe cheap, and actually has been involved in seeing it become a product by some kidney foundation. A cheap machine would help a lot, lots of people have to move to be close to the machines, or make long commutes that mean they have no real life.
Michael
I
But the problem with most organ donors, is they don’t donate their organs after they die…
they donate their organs and then die!
We joke, but our science may reach the point where we have an organ donor twin, all tanked and ready to go.
Not surprisingly, a common science fiction trope. A not-awful movie version is The Island: https://www.imdb.com/title/tt0399201/
@Ren – Citation Needed.
In fact it is hard to think of a comment where it would be any more appropriate than yours to reply “Citation Needed”.
It is incredibly irresponsible to spread such an idea unless one has a valid reason to believe it is true. Consider this, someone here could already be on the fence regarding organ transplantation. They could read that and it could be the last little nudge that pushes them to the ‘do not donate’ side. Depending on circumstance one donor can provide organs for several people in need. This means that it is entirely possible that several real people could die because of what you typed.
Now this is fine IF you can back it up. IF you have actual reputable sources you can quote (not dumbasses like those infowars blowhards). In that case you could be actually doing a service, informing people of a danger and perhaps encouraging people to fight to make things better.
I don’t think you do. I think you are repeating some BS you heard from a conspiracy nitwit and were too irresponsible to consider the potential consequences.
Now prove me wrong.
There is an alternative method that allows the patient to do the dialysis at home overnight while sleeping (or awake during the day – flexible), peritoneal dialysis, which does the filtering in the abdominal lining, the peritoneum. It does require some help, such as from a family member (with training), but does give the patient a lot more mobility, without the “time out” of hemodialysis at a medical facility. It’s not for everyone, but can be a more bearable option depending on individual circumstances.
Meanwhile keep hoping/praying for a stem cell breakthrough that would enable re-generating kidneys!
I slept through a lot of dialysis sessions, which started at 6pm. I said it was tedious, once the cinnectors are in place it just takes time.
I did read a few months ago abkut someone with a dialysis nachine in his basement, but no explanation of cost or how it happened. But it still used up his time. And seeing tbe process of hooking me up, a worry about infection, I do wonder how easy it is for the untrained to make the connection.
But, tgefe was a story two weeks ago about some smaller and relatively cheaper machines going North so people up there had access without having to travel or move, which is a great thing.
Michael
I think the problem with home dialysis is not so much the machine, which could be leased, or the hookup, which could be done by a visiting nurse or trained family member. It’s the massive volume of dialysate solution needed even for one patient. I forget where I saw it, but when I was researching this article I saw a picture “backstage” at a regional dialysis center, which had massive tanks of highly-purified water to mix with salt solutions to get a dialysate of the proper osmolality. Yeah, that’s to support dialysis on many patients each day, but even for one patient, creating enough dialysate from tap water would be difficult.
Now maybe if there were a dialysate delivery service, kinda like Poland Springs or something…
I never saw that, but maybe a tank was out of sight.
But there was small amounts of fluid, something fitting into tge machine but also bags of fluid like for IV except they fed the machine. And yes, something had to be run through it to clean it, and various external tubing tossed out after use. Plus a kit for cleaning my connectors, one before the hookup and one after.
It’s not an uncomfortable process, I often slept, but it’s an incredible burden.
I was lucky, it only went on for ten weeks, and tge chemotherapy rejuvenated my kidney “just enough”. They hope it will improve more, but time will tell.
Michael
I think this is the picture I found:

And those are just the concentrates – they have to be diluted with highly purified water to reach the final osmolality before being used by the dialysis machines. Granted, this is for a big unit with lots of patients every day, but the point stands – it takes a LOT of liquids to replicate what the kidneys can do.
One thing they been working on is to use a pig kidney as a replacement.
Two ways are being looked at first genetically modifying the pig to make it human compatible and the second they remove all the existing cells leaving just the scaffolding and seed it with human stem cells.
I saw an article once where they did this with a heart, it was washed of the cells, leaving a “framework” and then stem cells from the patient were used to grow new heart tissue, and the result was a heart that the patient’s body would not see as a foreign body and reject.
You mean like in this picture?
https://i2.wp.com/i.dailymail.co.uk/i/pix/2011/04/04/article-1372938-0B77D81700000578-132_468x286.jpg
And since you are left with just a collagen frame you could use a pig heart, structurally very similar to a human heart, seed it with human stem cells and (hopefully) grow a new human heart.
I recall an artificial bladder being constructed in a similar way about 10 years ago. I was interested, as the older method of stealing tissue from either the intestine or the stomach usually requires the patient to self-cath instead of having a functioning bladder; and the stomach tissue method that was practiced in the 90s has had a bad tendency of having the tissue lose pliability and cause reflux and kidney damage.
Discussing it with the head of urology at a teaching hospital after seeing the doctor, who developed the procedure, and the young man who received the first human implanted one give a TED talk about it, he said how he had read the original paper and been in contact with the doctor who developed it. Unfortunately, he informed me, the young man had already had to have a second bladder surgery, this time using the old intestine method; the neo-bladder from framework and his own adult stem cells had lost pliability in less than five years.
So the technology is there, but biology and human cells keep teaching us that there are things we think we know and are completely wrong
“Some teenager had a science fair project about making a dialysis machibe cheap…”
As a layman, I don’t see a technical reason why a dialysis machine can’t be cheap and more accesible. I mean a young doctor working during a wartime under, what must’ve been, difficult circumstances managed to build one from what look like a repurposed B/W print washer, a washing machine motor, and a pram. And this was 70 years ago. Surely technology have advanced to the point where we can make portable/carry-on ones, no?
AFAIK the problem is threefold 1. you need biocompatible material so you don’t accidentaly poison your patient from leached chemical or particles. also the membranes are a bit tricky they should allow for fluid transport and yet they should not break or cause other problems so usually those are kind of “hightech” materials. you could potentially do with simpler membranes like they used in the past but the efficiency would be worse.
2. everything has to be sterile(!!!) and since the machine is not one use it should be build i such a way that i can be made sterile easily. 3. the problem with portability is not the machine itself but rather the amount of consumables. remember you basically swap out old blood plasma for new “fresh” once so you need a few liters of solutions at least. also my understanding is that the pump is not really an energy saver so the battery-pack would be quite big since this has to run for a few hours at the time.
At least the energy problem would be quite manageable these days: Batteries from cordless tools are capable of several 100W and you could easily swap them during the operation of the machine, if necessary every 1/2 hour. It is not driving your heart, so I think if the machine stops for a minute during battery swap, it does no harm. If it would be a problem then you could still make two battery bays and swap them alternatively.
The difference is that during wartime, some 80 years ago, you could perform a lot of crazy experiments on people who were dying anyways, without worrying about killing them to infection because someone sneezed in the same building where you kept the machine.
Well, there was a case of patient who received his personal dialysis machine, back in 1950’s, IIRC. First case of both home dialysis and use of surgically implanted shunt to connect one to the machine ever. His wife had to prepare over 130 liters of dialysis fluid, pump cleaning and disinfecting solution trough the machine, plug her husband in and wait for cycle to finish. Then she sealed his shunt and emptied and cleaned the machine. IIRC, she performed these tasks 4 times a week for 18 years…
Three-letter answer:
F
D
A
Or insert your local regulatory agency here.
Sterility and liability.
Confronting them in reverse order: seventy years ago, if his patient died then at worst he hastened their death by a few days. Now days, that would be a lawsuit! If the pig intestine had the tiniest bit of bacteria and caused sepsis, if the saline got some stray chemicals like lead, copper, or chlorine (from tap water) or antibiotics (from tap water or hospital confusion in tracking) then the patient might end up in a bad place. At worst, a round of dialysis that doesn’t work, or absorbing some stray metallic ions that their liver isn’t able to handle.
To my understanding, once both kidneys are gone, the liver has been compensating for filtering things that aren’t urea for a while and is already stressed to nearly the breaking point.
Back to the first point, the sterility of the devices has to be impeccable. Blood left in the device has to be cleaned out thoroughly, because some could become a growth medium for infection, or some could clot and become a stroke, embolism, or heart attack waiting to happen. The filter medium has to be JUST H2O and NaCl in isotonic ratio; sure you can buy a liter of that at the drug store for a few bucks for rinsing eyes or cleaning cuts, but do you trust it to be 100% pure? Would you trust not just your life, but the life of a loved on to that sterility?
So I think it is very good, that we have the regulation in Austria, that everybody is a possible organ donor if he does not actively opt out. Man people do not really want to think about their death and the circumstances which make somebody become an organ donor.
“15 patients treated with it in Kampen, only one survived”
In today’s world, that’s 14 lawsuits. :-(
You get points off if you are already doomed to die. You are a bit more insulated from lawsuits if you are terminal, and there is nothing but the experimental stuff available.
Some more details about Kolffs artificial kidney:
1. To connect the rotating drum with cellophane sausage tubes, he had to find proper sealed axial connectors. He sourced them from Volkswagen, parts of fuel pump.
2. The machine was placed in room 13 of the hospital, Kolff changed it to 12A. Doors were very narrow, so to move in the first patient they had to break the wall next to the door.
3. Cellophane tubing was fragile and prone to breaks. When that happened, the blood would mix with the dialysis fluid, making it froth like crazy and spill out from the tub. For this reason everything in room 12A stood on bricks and there were few pairs of rubber boots waiting. One day, when Kolff was showing the dialysis to the people who ruled the region during occupation (to get more funds and help for his invention), cellophane ruptured. That didn’t help him much.
4. Kolff hoped that by reducing the levels of urea and taking the strain off of damaged kidneys, they will heal on their own. However most of his patients had kidneys too damaged to heal. One of his patients however got a bit better with artificial kidney. Kolff used glass cannulas to connect his patients with the machine. In case of that patient he ran out of blood vessels he could insert cannulas into before she was healthy enough for her kidneys to work again. This problem prompted the invention of surgically implanted shunt in later years.
The whole story of artificial kidney and other breakthroughs are described in book by Jurgen Thorwald, “Patients”. He has entire series of books on history of medicine and especially surgery.
That’s great detail, thanks so much! I tried to find more information on how Kollf connected the patients to the machine, and finally decided that he must have treated the blood in batches before returning it to the patient. But I guess you wouldn’t be able to pull more than a liter out of a patient at a time to treat, so it wouldn’t be a useful process.
I’ll have to pick up that book, sounds fascinating. Thanks!
He ran the machine for many hours, cleaning 60, 80 or more liters of blood in one go…
Hopefully this will educate and dispel any misconceptions.
I am currently on hemodialysis. I sit in a chair at a center for 8 hours (three nights a week). The “normal” 4 hours did not work for me. I am listed at three transplant centers. Waiting…
The dialysis machine that sits to my left is a life saving device. It does a whole lot more that just pump blood through a filter (called a dialyzer). It can administer medications (like heparin) and puts saline back into the blood.
There are three ways to do dialysis:
1. Hemo, in a center.
2. Hemo, at home.
3. Peritoneal, at home.
Each has its pros and cons from my perspective.
I started out three years ago doing peritoneal dialysis at home. I would hooked up to a machine for 9-10 hours. I slept through most of it no problem. I had to attach/detach myself to the machine (cleanliness is SO important here) using a catheter that hung out of my belly. To do this type of dialysis you need to have room for the 35-40 boxes of solution that come every month, plus A LOT of other supplies. After getting an infection (I told you cleanliness is important). I had to have my catheter removed and switch to hemo dialysis.
There are three types of hemo dialysis access (to your blood):
1. A fistula with needles in your body every treatment
2. A artificial graft with needles in your body every treatment
3. A catheter in your chest (kind of like for chemo), that provides external plumbing that can plug/unplug each treatment.
I’m rambling.. but check this out:
https://pharm.ucsf.edu/kidney
My thanks to Dr. Kolff. His work saved my new born sons life. At the tender age of 3 days, my son was put on an ECMO machine for a week. ECMO = Extra-Corporeal Membrane Oxygenator. The device basically was attached to the carotid artery and was used to reoxygenate, warm, and then pump blood through his body so that his heart and lungs could rest and recuperate. Quite the nerve racking experience seeing your son on this type of device. He survived and is doing well. He has my thanks.
Thanks for that story!