Preterm infants frequently require ventilator support while they’re in the neonatal ICU, and this is usually done with a CPAP machine. The machine to infant interface is called a nasal cannula, a bit of plastic that connects an infant’s nose to the machine. Because there aren’t that many sizes of nasal cannula available, and preemies come in all sizes, there are inevitable problems. Ill-fitting nasal cannula can reduce the effectiveness of a CPAP, and can even cause significant damage to an infant’s septum.
For his Hackaday Prize entry, [Ben] is tackling this problem head on. He’s working on creating individualized nasal cannula for newborns using 3D modeling and printing, allowing nasal cannula of all shapes and sizes to be created in a matter of hours.
To create these customized cannula, [Ben] is 3D scanning an infant mannequin head to gather enough data to import it into a Processing sketch. A custom cannula is then created and printed with flexible 3D printer filament. In theory, it should work, apart from the considerations involved in building a medical device.
As for why custom plastic tubes matter, [Ben] works at the only NICU in Western Australia. Even though he only sees 8-10 CPAP ‘pressure injuries’ in his unit each year, these kids are extremely fragile and some parents have expressed a desire for something that isn’t as uncomfortable for their newborn than the off-the-shelf solution. Customizing these cannula from a quick 3D scan is a great way to do that, and a perfect example of the Hackaday Prize theme of ‘build something that matters.’




















Awesome!
I guess 3d printed parts come out sterile too, due to the heat involved in printing them?
Urine comes out sterile as well… you’d also need a sterile 3d-printer, handling equipment, etc.
Then, comes the other stuff like chemical residues.
Urine in and of itself is sterile, but it does not come out of the body in a sterile state due to bacteria on/in the external plumbing so to speak.
The :urine is sterile” mantra is like the it’s the “amps that kill not the voltage” mantra. Both are true as far as they go,but are incomplete information.
Apart from the considerations of making a medical device!
Which are huge, much of which will ensure that it cost orders of magnitude more than now. Lawyers have to eat too. They don’t at Micky-D’s though.
I doubt direct 3d printing of flexible materials from a deposition printer is ever going to get medical certification. There is just no way to get all the residual gasses and surface contaminants out/off. Printing a mould for fast cure silicone however might just work. Any contamination would be on the surface and should probably evaporate on the curing bake.
You can always dip coat it in a silicone conformal coating. There are many that are FDA approved and the cure time is in minutes.
NICU person here — CPAP prongs don’t need to be sterile — it’s not like the baby’s nostrils are sterile.
The bigger issue I see is that the prongs are typically very soft and flexible, to reduce the skin breakdown. The standard PLA 3D prints I’ve seen are pretty hard. Is it possible to 3D print something that would be nice and squishy? If so, as a neonatologist, I’d be *very* interested in customizable nasal CPAP prongs.
Our patients on CPAP range in size from ~700 grams to ~5,000 grams, and the CPAP sizes don’t always work. Also, when we start to see skin breakdown, we’ll start switching between different CPAP interfaces (different prong types, vs. little ‘masks’ that cover the entire nose), just to change the pressure points around, even if the pressure delivery suffers. Printing up slightly different prongs would probably allow the pressure spots to move, while still allowing better seal / pressure delivery.
I think this is awesome.
There are flexible filaments out there. One of the well-known ones is Ninjaflex. You can get an idea of what it’s like from this video:
https://www.youtube.com/watch?v=ZnJZTwrQcQI
Thanks JC – I have been using NinjaFlex which is quite flexible but quite a pain to print. There is a shot in the first video of me flexing a printed model that was made using the processing template and vernier input. But it is a bit harder than the soft silicon these things are usu made from – not too far off though. I have sourced a locally made TPE filament (like NinjaFlex). It’s made locally in Australia (Melbourne), about half the price – but appears to be quite a bit softer. I have a roll but haven’t posted anything yet as it is even harder to print than NinjaFlex. Have modified my printer extruders for flexible filament but this new stuff is so soft it still finds a way to wrap around the drive gear. I’ve got a few plans – will see if I can get it to print. I also plan to modify the design to distribute the load over a greater surface area of the face – so I’ll ditch the cylindrical design and try to model a flattened triangular design. So should end up with a flat surface (from a facial scan) that spreads load across the face???
The other important point in your post is regarding skin breakdown. Outside a NICU this may sound undesirable but nothing too major. As I’m sure you understand more than I – these infants are so prone to infection that any breakdown in skin integrity can be a prime site for infection. And for a preterm infant – an infection can easily end a life.
Thanks for your comments.
Yep, you are right on the money. The TPU print is slow as molasses. Perhaps printing in ABS as a mold for silicon?
I would have thought t they would have been Medical grade tubing and a “Y” branch fitting. Allowing the use of tube for each nostril to deal with that variance, “whittling down the OD to fit that dimension.. Where the baby will have air delivered to it’s lung through the tube it would be important that the ID would be sterile
I like the idea regarding different sized tubing for different sized nostrils – I am still considering this as an option – the spacing between is also critical. I didn’t see this as a particularly practical option. And maybe 3D printing won’t be either – I’ll see how I go.
Don’t get too hung up on ‘sterile’. We obviously want the device to be extremely clean, if not sterile. However don’t forget that these devices are used for quite long periods of time. Even if it comes out of a packet sterile – the second it touches the baby it is no longer sterile. It’s going to sit in the nose (full of bacteria) in a warm moist environment for in some cases weeks – these devices are NOT sterile when used.
You can carry a baby for ~9 months, then care for it, school it, then it grows up, gets old, dies and goes to God.
Or you can abort and send your child to God the instant way. It’s up to you.
What does this have to do with Abortion?
Don’t feed the troll.
Which god are you referring to? Man has invented quite a lot of them.
Anesthesiologist here. Seriously, as this is supposedly the future and I use a 3D printer myself, where does the law stand on personalized devices like this? A maxillofacial surgeon can have a 3D printed metal plate made and implant it into someone’s skull with attendant press releases and so on. At a more basic level, an obscure airway some of my colleagues use has now ceased to be manufactured and they ask me if I can 3D print some for them. My answer is yes no problem but whether they would ever be allowed to use the printed part is another matter indeed. As with the CPAP prongs, it has to be clean but it does not have to be sterile, so as 3D printed medical gadgets go it is potentially a very good candidate for this kind of technology.
I don’t know where the law stands but if you use the 3D printer to print a mold (I just sent a sample to Ben) then you can fill the mold with medical grade silicone and have a medical grade appliance.
Routine sterilisation procedures will, of course, apply.
In most parts of the world – I.e. not the USA, how a thing is made is not a reason to not make it. Even in the USA, medical experimentation that saves lives is still acceptable.
But I suspect your question is more about your personal liability – which in the USA is a whole minefield of enormous size. Consult your medical insurance professional…
Big thanks to neon22 for the openSCAD scripts and model – will be taking a look at these – slightly put out you made more progress in a few hrs than I have in months ;) Just to add to these comments about 3D printing medical devices and legality/liability. I completely agree and see all the potential issues to get a solution like this to market. But there does seem to be a need – certainly getting a lot of positive feedback from clinicians. So I guess I could acknowledge all these problems and sit on my hands, or just have a crack – try to build a bit of momentum and demonstrate the possibility? In my experience regulators are willing to consider novel technologies and work with industries committed to ensuring safety – I’ve got some experience in this. Sure I may never get there, but I intend to have a go.
Thanks again for your help neon22 – will no doubt be in touch.
Ben
What a great idea.
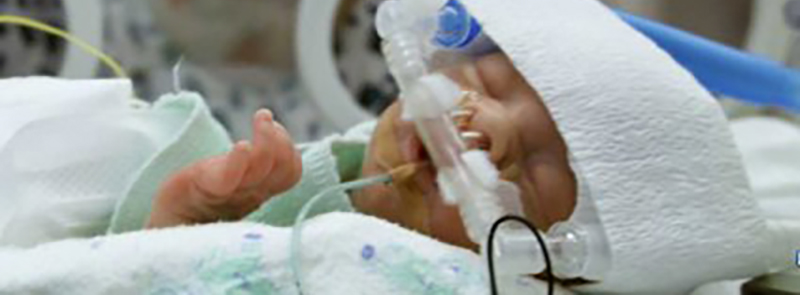
Judging by the photo atop this article, it looks like the plumbing is awkward and oversize too. Maybe a custom approach could also result in better-fitting system that’s less likely to shift position or apply inappropriate pressure.
Don’t they have neonatal nasal pillows? It’s one of the more comfortable nasal CPAP fittings for adults, and I’m not aware of any reason it couldn’t be scaled down.
Abortion is faster.
You act like a zealot, all zealots are insufferable. Clearly you aren’t pro-choice, because you act you don’t agree with the choice going through with premature birth.
Love the idea, but isn’t is possible to build the CPAP prongs to be tapered to a point and cut to match the nostril size of the infant?
Some of the existing devices are tapered (not sure if they are cut to appropriate size though). You’d probably need a range of sizes to cover the full range these infants come in. The 2 areas of damage caused by the existing device are at the septum – where it meets the upper lip – ie right between the nostrils. And way up inside the nares at the end of the tubing – where these ends move around they also can create scarring inside the nose. So I’m trying to do away with any excess tubing up the nares. This is not clearly evident in the current models as my starting point has been to try to model the existing device in Processing – then modify the problem areas. It’s very much an iterative approach because I am learning how to do this from scratch. I expect the finished ‘product’ could well look quite different from the current models shown on hackaday. Thanks for the input thought – it is great to suddenly get some extra help.
As the proud father of a preemie born 2 months early via emergency c-section at only 990g (2lbs 3oz), where he spent the first 2 months of his life in an incubator I say this is a great idea. Seeing our and other babies, barely able to touch them, hoping the best and seeing all kinds of sores and unintentional injuries anything that assists the process is a wonderful idea.