When auditory cells are modified to receive light, do you see sound, or hear light? To some trained gerbils at University Medical Center Göttingen, Germany under the care of [Tobias Moser], the question is moot. The gerbils were instructed to move to a different part of their cage when administrators played a sound, and when cochlear lights were activated on their modified cells, the gerbils obeyed their conditioning and went where they were supposed to go.
In the linked article, there is software which allows you to simulate what it is like to hear through a cochlear implant, or you can check out the video below the break which is not related to the article. Either way, improvements to the technology are welcome, and according to [Tobias]: “Optical stimulation may be the breakthrough to increase frequency resolution, and continue improving the cochlear implant”. The first cochlear implant was installed in 1964 so it has long history and a solid future.
This is not the only method for improving cochlear implants, and some don’t require any modified cells, but [Tobias] explained his reasoning. “I essentially took the harder route with optogenetics because it has a mechanism I understand,” and if that does not sound like so many hackers who reach for the tools they are familiar with, we don’t know what does. Revel in your Arduinos, 555 timers, transistors, or optogenetically modified cells, and know that your choice of tool is as powerful as the wielder.
Optogenetics could become a hot ticket at bio maker spaces. We have talked about optogenetics in lab rodents before, but it also finds purchase in zebrafish and roundworm.

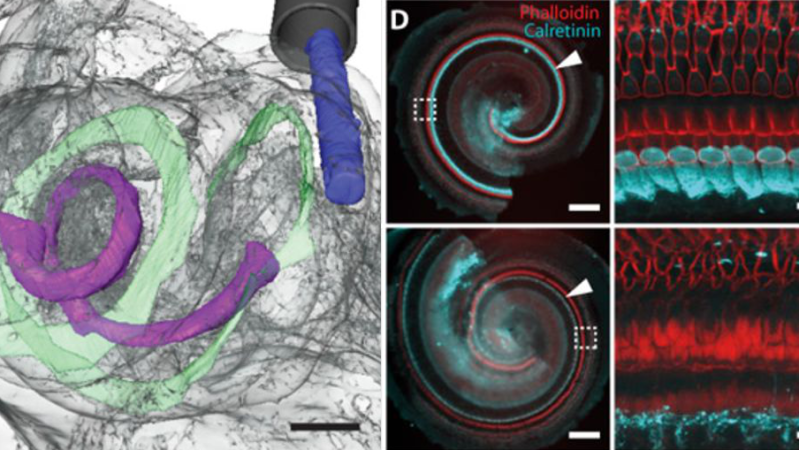














This is all very nice, but coming from the field, there is a huge issue with this kind of research: Current CIs work! They are based on electrical stimulation and users are generally happy. They often fail to allow enjoying music and directional hearing. The latter won’t be solved by optogenetic stimulation, the former might. However, the problem is: neither the viral transduction of cochlear tissue nor long term expression of light sensors can be considered safe. Nobody knows what happens after 40 years of foreign protein production in these cells! In addition, the required light emitting device is extremely difficult to make. Current CIs are based on hand assembled arrays of platinum wires. They take forever to make and are super expensive. Why? Because so far they are the only thing robust enough to conform to the required medical requirements! The manufacturers won’t even exchange them with (fancy) flexPCBs, just because of the risk. Nobody is going to put LEDs encased in flexPCBs into peoples ears anytime soon. There is no demonstration of sufficient long term stability and mechanical robustness. Plus, nobody knows whether they can really cash in on their higher resolution or whether the distance to the sensitized cells or scattering are going to nullify the benefits.
Therefore, a POTENTIAL small improvement of hearing might have to be bought at an insane price. It’s at best unrealistic to sell this story to people as the future of hearing aids and at worst unethical and a ploy to get research funding.
If this were for something for which no current treatment exists – okay- But not for something where even today fairly well working, safe treatments exist.
tldr: way oversold, tons of risks, not going to happen anytime soon.
Things move forward with time. I was once hired by a prosthetic company to design tactile/visual aids for profoundly deaf infants, and there was a decent market at the time because it was CI’s that were _extremely_ iffy, and infants needed something pretty much right away to not feel totally abandoned when mom left the room. The surgery for a CI was neither easy (is it now? That’s a hard spot to get to!) or cheap, and failure to understand some things meant they essentially burnt out some neurons over time, if they didn’t just fail themselves (and replacement costs, see above). Just sayin.
Almost everything isn’t as good at first as it will become if it was a good idea.
CI’s at that time sounded at best like “banging trashcan lids together” (quote from a user who had once had normal hearing) – what a way to experience life!
I agree. But what people don’t understand is that the difference between electrical and optogenetic CIs is not between bicycle and car to get from one side of town to the other, but between bicycle and teleporter. Might happen some day, but most people prefer the bicycle.
What you describe is the situation before any reasonable treatment. Modern CIs are pretty good and very safe. If you were deaf, what would you prefer:
1. safe procedure to likely get back the ability to communicate effectively with other people for the rest of your life and the potential to get an even better implant in the future
2. totally unknown procedure that might cost you any chance of ever hearing again with any technology to >maybemaybe< enjoy music to some degree as well.
Some people are desperate enough to risk anything to get their hearing back, even to the point of risking permanent damage from experimental procedures.
On the one hand you will be able to communicate verbally but never enjoy music again. On the other it’s a gamble but if it goes well you may get both?
Well… some people’s priorities might be different than yours. I’ve never met a person that doesn’t listen to music at all but some definitely appreciate it more than others. For some music is their main passion in life. I think they should get to make their own choice as the risk vs benefit ratio may be very different for one person than it is for another.
It’s easier to use already developed technologies so stop developing new ones?
It took a lot of trial and error to get where we are today too. Progress is never free. Perhaps we should have stopped with pointy sticks and stone hand-axes?
” Nobody knows what happens after 40 years of foreign protein production in these cells! ”
At one point nobody knew what happens after 40 years with a CI. What is your point?
You hear light, to answer your question, since they are auditory cells.
Public service notice:
I’m a 60-something male. Two years ago, I woke up one morning, feeling like one ear was full of wax. Couldn’t clear it. Couldn’t hear a damn thing out of it. I was seeing a ENT doc for something else, so I went in to see if he could clean it out. Instead, he told me I had Sudden Sensory-Neural Hearing Loss in that ear and the prognosis was uncertain. He put me on a two-week course of steroids, which is the only treatment, and it’s only effective if you get it within about 48 hours of losing your hearing. Apparently, this is something that happens to people in their 60s, and it’s usually only in one ear. Tell your older friends, it may mean the difference between deafness in one ear or being able to hear. Let me tell you, it’s terrifying to be totally deaf in one ear.
The reason I’m posting this here, is that I got my hearing back (and I have the before and after hearing tests to prove it), and you can too, but only if you act quickly. Here’s the test to see if you have wax or SSNHL: Hum. If you hear yourself humming in both ears, you’re good, clean out the wax. If you only hear humming in one ear, GET YOURSELF TO AN ENT EMERGENCY ROOM! Luckily, I was seeing this doc for something else, and I’m in Boston, so we have loads of great medical resources.
No one knows what causes SSNHL, there is suspicion that it’s a virus, but no proof, and having had it, does not mean you’re any more likely to get it again. More information here: https://www.masseyeandear.org/for-patients/patient-guide/patient-education/diseases-and-conditions/sudden-deafness
Thank you!
I had never heard of SSNHL
(I would have thought it had to do with the National Hockey League -tongue in cheek).
No, the symptom of that would be a sudden loss of teeth, not hearing.
Good to know. I’m just a few years from the age where this might be an issue.
You’re welcome. I’m somewhat of a celebrity at the ENT doc’s office…I guess they see this occasionally, but saves like mine are rare, because people don’t get treatment quickly enough. They are very happy to have been able to see it cured. Even the doc was somewhat excited (he’s usually very sedate)
It’s all a bit surreal, I almost wonder if it really happened. My hearing is back to normal now. But I’m well aware that I dodged a bullet. The two weeks while I was waiting to find out if the steroids would work was terrifying (meetings at work were very tough — I was wondering if I would still be able to work).. And feeling the hearing come back over the course of the third week was even weirder…at first, it was like a busted speaker, just weak bursts of noise in response to very loud sounds, then, gradually, like I was tuning in a radio station, the sounds got clearer. I didn’t dare think that it would get better, lest I jinx the recovery. Coming down of the hefty steroid dose was fun on its own — headaches and such.
So, please spread the word. It’s another one of those things that if you have knowledge, you stand a better chance of coming out ahead.
my daughter was born with hearing loss but with thw help pf hearing aids she is almost fine but with the passage of time her hearing is decreasing. may be due to wax or mucus in her ear.. i want to know tqo things
is there any treatment for such hearing loss
how to improve her hearing decreased due to wax or mucus due to flu etc
So its a semi-biological opto-isolated hmi, now just get sub-vocals out and I can have Siri/alexa/cortona/joi in my ear for company 24/7, sign me up…
But my serious question would be since the sounds are now being sent via light could you replace the sound data with visual data and have the brain interpret it? similar to the low resolution sight given to blind people through an electrode on the tongue experiments that have been going on for years now and I seem to recall a cochlear style implant for vision being tested about 10 years back.
Doing a rough search I find lots of experimental devices & procedures to correct deafness & blindness and despite varying degrees of success but nothing ever seems to develop beyond the experimental stage.
I enjoyed your post. I wear a BAHA and love it. It works much better than hearing aids and the clarity is amazing.