One of the most critical skills in emergency medicine is airway management. Without a patent airway, a patient has about four minutes to live, so doctors and paramedics put a huge amount of effort into honing their intubation skills. They have to be able to insert an endotracheal tube quickly and efficiently, without damaging sensitive structures like the vocal cords. It’s a tricky skill to master without a ton of practice.
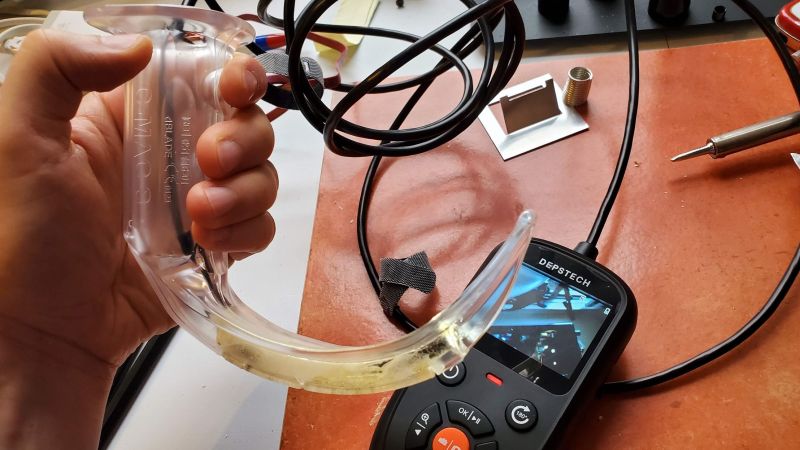
The perfect tool to practice these skills is a video laryngoscope, but these are wildly expensive and reserved for clinical use. Luckily, with a little ingenuity and a cheap USB borescope, [Dr. Adam Blumenberg] and [Dr. Erin Falk] were able to come up with this low-cost video-assisted laryngoscopy setup to reach as many students as possible. The idea is to use a single-use laryngoscope blade, which replicates the usual tool used to visualize the patient’s vocal cords. The blade is made from clear plastic, which makes it perfect for the application. The borescope is passed through an opening in the blade and affixed to it with adhesives. A little Dremel work might be necessary to get the optical axes of the blade and the camera to line up; failing that, there’s always the option to disassemble the camera to get a better angle.
The chief advantage of this setup, aside from being cheap, is that it’s something that it’s not intended to be used on patients. Along with an airway manikin, the tricked-out borescope can sit in a conference room waiting for students to have a go. Using a large screen allows the whole group to watch the delicate procedure and learn from the mistakes of others. It may not be as detailed a simulation environment as some, but “blade time” is really what counts here.















At first I thought this was going to be about placing an NG (naso-gastric) tube post pyloric (into the duodenum).
Manikin eh? Step up from practicing on each other, or borrowing grads from another department.
As one of those (ex)paramedics who put effort into keeping these skills honed, I can tell you this isn’t a procedure you’re going to rope an unwitting volunteer into.
On a TV show recently I saw medics using a laryngoscope with a built-in borescope and mounted screen. I would think this would soon become a norm to reduce the medic’s contortions and to improve visualization in those fringe cases where you just can’t get a good view of the cords.
I see the value of this particular invention in the ability to throw it on the big screen; the ‘learn from other’s mistakes’ part of it.
The device in the picture looks freaking scary and the idea that somebody puts this into me makes me shudder, but i guess when you are about to die you don’t care… Thanks to all paramedics and doctors and nurses and so on.
I’ve worked for two private EMS companies, they both have video laryngoscopes on all Advanced Life Support trucks (the ones that sometimes have “Paramedic”, or “ALS” on the sides). Interestingly, quite a few medics hate them. I don’t think I’ll be one of those medics.
One of the companies actually has a manikin and a video laryngoscope in one station so crews could train. It would be really handy to have access to that right now, but, if I had access to it, I wouldn’t be able to afford paramedic school because the wages there were quite poor (but not the worst in the state, one place pays nearly minimum wage for EMS-D)
I know nothing on the subject, but seems like a nicely done cheap practise equipment. Good stuff.
Great idea but I wish there was a way to attach a thinner light tube or fiber to the borescope as even the 5.5mm ones are a bit big. I find I can’t get them very far into my nostrils.
I’m a physician and intubate people all day, every day.
Couple of clarifications for the article- one is that yeah if you don’t breathe for a few minutes it is indeed bad/fatal, but placing a true “emergency” tracheal intubation airway almost never happens, either in the field or in the OR, ER or anywhere else. To explain a bit further, the first step is always mask ventilation, which is adequate (and often better) in a number of ways. I frequently tell learners “good mask ventilation saves lives, bad intubation ends lives.” With good mask ventilation, you usually have allll the time in the word to calmly and without fanfare place an endotracheal tube. Exceptions are a true “difficult airway” (that has a very specific technical definition, not the layperson definition) or massive vomiting or some other reason that masking isn’t possible.
It doesn’t actually take a “ton of practice” either, any more than any other medical procedure. I regularly teach medical students to safely place them in a day, but the vast majority of the teaching is the algorithm for placing, how to trouble shoot, when to know if you are in or not, that sort of thing then rather than the mechanical skill itself. But, like anything, those that do it all the time (OR/ER staff) are much smoother at it than learners or, say, flight nurses that don’t do it very often and need refresher training. See above re: good/bad intubation.
The dummy for training is super expensive, like $1000 or something I guess because it is specialized equipment, not a huge market. The videolarygoscopes are everywhere, and when we teach workshops and stuff we just take one from the OR and use the “real” one. Anywhere that has and ER, or ORs has them now, they are quite common, even though I’d still bet like 90% of OR intubations are without a video ‘scope, it is done with “direct laryngoscopy.” So finding a scope is the easy part, the dummy is the hard thing to find and learners are hard on them too!
I hope this helps… someone. Best.