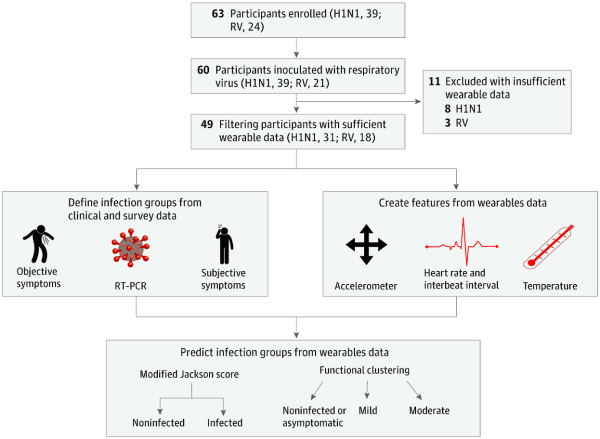
Sometimes we dig through the archives to see what kind of crazy hacks we can pull out of the depths of the world wide web and this one was worth sharing. Researchers at Northwestern University developed a sticker that’s applied to the fingernail and measures heart rate, motion, and blood oxygen, all without a battery.
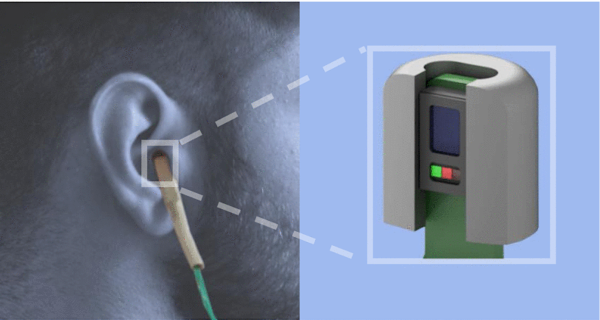
The photoplethysmograph (PPG) system is similar to what we’ve covered before and the motion sensor is simply an accelerometer, so we won’t go over those aspects of the device. The parts of the device that did catch our attention were the battery-less operation as well as its size. It’s just so dang small! And fits snuggly on a fingernail or on even on your earlobe. The size here is actually a very interesting feature and not just a marketing plug. Because the device is so small and lightweight, it is very easy to adhere to the fingernail or skin with very little sensory perception. Basically, the person wearing the device won’t even notice it’s there. That’s definitely an advantage over the traditional, bulky, hospital-grade instruments we’ve grown accustomed to.
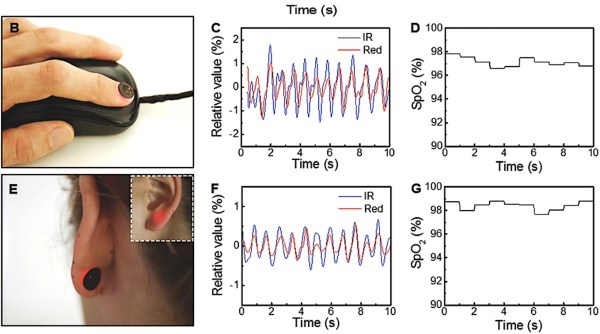
The device adheres really well given its small and lightweight design, so motion artifacts are significantly reduced. Motion artifacts in PPG-based devices are due to the relative motion between the optode (LED and photodiode) and the skin. The traditional approaches of ensuring the device don’t move are for the patient to keep very still during a recording, to wear the device tightly against the skin (think of how tightly you need to wear your smartwatch to get consistent readings), or use some seriously tough and uncomfortable adhesive as you may have done if you’ve ever gotten an electrocardiogram reading before. This device eliminates those three problems.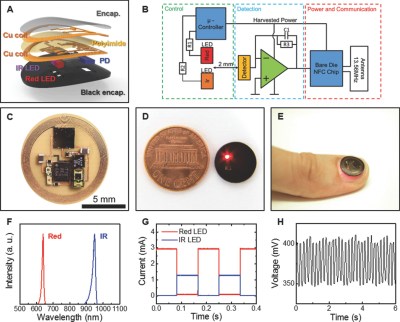
The other aspect of the device that caught our attention is its use of wireless power instead of a battery. In some senses, this could be seen as an advantage or as a disadvantage. The device relies on NFC for power and data transmission, a pretty common approach for devices that only need to be used intermittently. Wireless power could be a bit problematic for continuous monitoring devices which provide readings every second or several times a second. But who knows, wireless power seems to be everywhere these days.
Digging into the details a bit, the double-layer antenna is designed around the circumference of the device using wet etching to create traces on a copper polyimide foil. The team electroplated holes through the different layers of the device (optode layer, first antenna layer, polyimide, second antenna layer, component layer, protective top coat) connecting the antenna to the die pad NFC chip (SL13A, AMS AG). Connecting the chip requires some pretty fine-pitch soldering techniques, but nothing we’re not accustomed to here at Hackaday. Overall, they seemed pretty successful, obtaining a Q factor of 16 and a transmission distance of 30 mm using a smartphone and not some giant reader antenna.
Definitely, a really cool project that we recommend checking out.

 Their device includes a number of components we’ve seen already. There is an HC-05 Bluetooth module,
Their device includes a number of components we’ve seen already. There is an HC-05 Bluetooth module,